More than a decade ago, we introduced a five-step framework to help life sciences companies build pull-through capabilities that communicate cost and coverage realities to prescribers.1
Figure 1: Original 2014 pull-through capabilities five-step framework
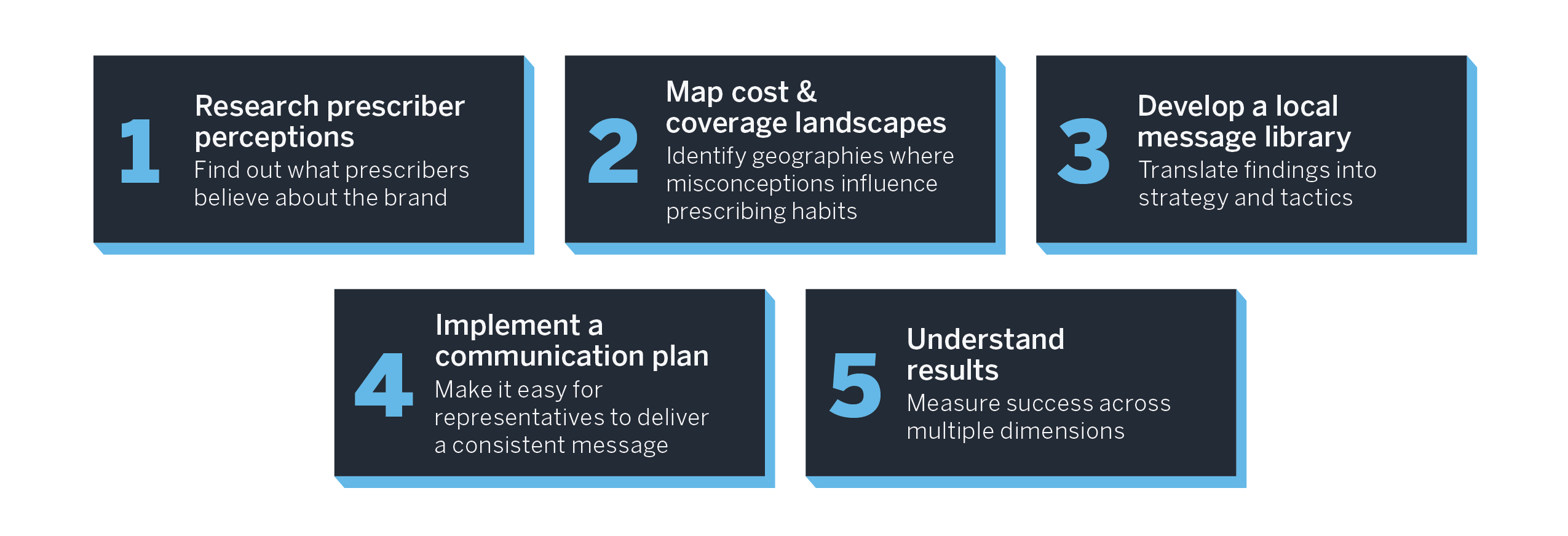
These core pull-through challenges have not disappeared. Prescribers still face limited time, fragmented coverage, and lasting impressions from prior access experiences. What has changed is the speed, variability, and operational complexity of the ecosystem surrounding those decisions.
Today, four key forces are reshaping the access environment prescribers must navigate:
- Policy and market changes have altered the access landscape. Medicare redesign, drug price negotiation, the growing presence of biosimilars, and direct-to-consumer (DTC) distribution models have all increased the operational complexity of prescribing and patient access.2–5
- Technology and data capabilities have advanced dramatically. Digital platforms now allow organizations to reach targeted audiences with greater precision across multiple channels, and artificial intelligence (AI) and large language models (LLMs) have transformed how organizations interpret data and deliver insights.6
- Industry operating models have also evolved. COVID-19 accelerated the adoption of digital engagement and reshaped field force strategies. Contracted sales teams are more common, and access to healthcare provider (HCP) offices continues to tighten.7,8
- Therapeutic complexity has increased. The growth of specialty therapeutics (e.g., treatments for rare diseases, immunotherapies, and other high-complexity products) has made prescribing and patient access more individualized, increasing the need for precise, indication- and patient-specific pull-through support.9
Together, these changes make it worthwhile to revisit and refresh our original blueprint, as outdated pull-through strategies can no longer keep pace with how access barriers emerge, shift, and affect prescribing decisions. When cost and coverage guidance is too broad, too slow, or insufficiently local, prescribers and practice staff are forced to rely on past experience rather than the current access reality, creating friction for patients, misaligned treatment decisions, and delays or complications in the access process.
A five-step approach to pull-through in the modern pharmacy access environment
The modern pull-through priority is no longer simply communicating cost and coverage information; it is turning increasingly complex access realities into clear, actionable guidance at the point of prescribing. Doing so requires a pull-through capability that is insight-driven, locally relevant, operationally integrated, and measurable over time in ways that utilize the modern technology and data capabilities at hand.
The following five steps are the updated foundation for building an effective pull-through capability.
1. Research prescriber perceptions with modern and synthetic research approaches
Prescribing decisions are still driven first by clinical judgment, not by real-time access visibility. Even as awareness of affordability and utilization management has increased, most providers and their staff are still making decisions without a complete view of what a specific patient is likely to face at the point of access. Gathering insight into these perceptions remains the first step in building pull-through capability.
Traditional research methods (e.g., advisory boards, in-depth interviews, pulse surveys, and research panels) are still critical for understanding how prescribers and practice staff perceive the access landscape for a therapy and its alternatives. These methods can help uncover the beliefs, assumptions, and prior experiences that shape prescribing behavior, particularly in environments where coverage restrictions and patient affordability vary widely.
However, what has changed in the last decade is the ability to translate those insights into more refined HCP profiles and to test engagement strategies more dynamically. Rather than relying on a generalized “average prescriber,” organizations can now use data to define panels or create HCP archetypes that reflect meaningful variation in access experience, including payer mix, coverage friction, practice setting, workflow maturity, and roles in access decision making. Once the panels with diverse personas have been designed, strategy can be tested for a better understanding of how pull-through needs may differ across provider types, practice models, and local market realities.
Synthetic research is another developing capability that can complement this work, using AI-enabled models and simulated HCP scenarios informed by real-world research findings to test and refine messaging and access-related engagement more quickly than traditional research alone. Both HCP profiles/panels and synthetic research can help organizations evaluate how different populations may respond to access messaging, support resources, and engagement pathways before broader deployment.
These more modern capabilities should be used to generate hypotheses and refine engagement approaches, but they should not be considered a comprehensive replacement for primary research with HCPs and practice staff. Traditional research methods remain a critical step in this process; when traditional research methods are used in conjunction with synthetic research approaches, organizations can build a more nuanced understanding of prescriber perceptions and design pull-through strategies that better reflect the full range of access realities encountered in practice.
2. Map access landscapes and opportunities by identifying where misconceptions influence prescribing habits
Access conditions can no longer be generalized at the national level. They vary across micromarkets based on payer mix, utilization management, patient population, and local practice dynamics, creating environments where prescribing behavior may lag behind current access reality. Mapping these access landscapes helps identify areas where misconceptions about cost and coverage are driving that gap.
Modern analytics and AI capabilities make this process easier to access and act on by translating complex data into clear, usable insights rather than relying on static spreadsheets or manual dashboards. These tools allow organizations to evaluate access conditions at the micromarket level, helping teams distinguish between two factors that often become blurred together: (1) what is true locally about access and patient cost, and (2) what prescribers believe is true based on experience.
When prescriber perception and data-driven access realities are mapped and compared, patterns of misconception become visible. A practical approach is to segment micromarkets based on relevant access conditions, such as payer mix, the level of coverage requirements (e.g., prior authorization or step therapy), rejection or abandonment patterns, and practice setting. These segments can reveal unexpected underutilization pockets (i.e., markets where access appears favorable or improving, yet prescribing remains below guideline expectations or peer benchmarks).
These situations may indicate that outdated experiences or incomplete information is shaping prescriber perceptions. Identifying these gaps allows organizations to focus pull-through efforts where correcting misconceptions is most likely to change prescribing behavior.
3. Develop a local engagement strategy that includes ongoing training and targets underutilization
Once perception gaps and access opportunities are identified, organizations must translate those insights into practical, ongoing training for the field.
Training must be:
- Execution-focused: Teaching what to do when specific barriers arise (not only what they are)
- Scenario-based: Practicing common situations (e.g., prior authorization, step therapy, specialty pharmacy routing) with clear next steps
- Measured: Evaluating against a baseline and refreshing training based on observed gaps
- Reinforced over time: Delivering regular refreshers, reminders, and feedback loops (weekly/biweekly where feasible)
From a tactical perspective, pull-through efforts must address two common drivers of underutilization: (1) knowledge gaps and (2) misperceptions about access. Local data and signals (e.g., utilization patterns, time to therapy, field feedback, etc.) can help diagnose which of these factors is most relevant in each market, increasingly with the help of AI and automation.
For example, an AI-powered dashboard can flag accounts where local access is improving but utilization remains low, while an AI chatbot interlaid with business intelligence and compliance frameworks can answer, “What should I do next,” with market-specific talking points, objection handling, and the appropriate referral to reimbursement or patient support resources. Employed concurrently with the other approaches outlined in this paper, these tools can help field teams translate access insights into more targeted and timely engagement strategies.
Pull-through efforts must then deliver customized access guidance that reflects local conditions and enables providers and their staff to move from barrier identification to the next practical step. This may involve education, support programs, reimbursement resources, or patient services, but in all cases, engagement should be tailored to the specific access environment. When guidance is accurate, role-relevant, and locally grounded, it helps reduce friction in the prescribing process and supports patients in moving forward to therapy.
4. Integrate the pull-through approach across the pharmaceutical access journey
While pull-through is often associated with messaging, the broader objective is to support the full patient and provider access journey.
One way to view this process is through a funnel that reflects the potential stages between awareness and successful therapy use:
- Awareness
- Intent to prescribe/prescriptions written
- Payer rejections
- Patient abandonment
- Therapy initiation
- Adherence
Applying this framework across national, regional, and local levels helps identify where patients and providers encounter friction.
In the original framework, the funnel was primarily used as a conceptual model. Today, organizations can anchor each stage to observable signals drawn from operational data, such as claims and utilization patterns, rejection and abandonment trends, hub and support program activity, field observations, and local coverage conditions. These signals provide a clear view of how patients and providers move through the access journey.
Used in this way, the funnel becomes a diagnostic tool rather than a performance scorecard. Early-stage drop-off may suggest low confidence in coverage conditions or incomplete understanding of access pathways. Midfunnel friction, such as rejections or abandonment, often points to operational or affordability barriers. Later-stage gaps in initiation or adherence may indicate challenges with support activation or patient follow-through.
This diagnostic approach helps organizations determine where pull-through efforts should focus. Rather than building new programs for every challenge, teams can adjust the emphasis of existing capabilities (e.g., training intensity, pathway clarity, field or staff enablement, digital reinforcement, or support program visibility) to address the most significant sources of friction.
5. Understand results by measuring success across multiple dimensions
Modern pull-through measurement should assess not only whether engagement occurred, but whether it changed behavior, shifted access perceptions, and reduced friction in the parts of the journey where support matters most.
Three dimensions remain especially useful:
- Direct impact: Effective pull-through efforts should influence prescribing behavior when access conditions are relevant. Advances in claims, coverage, and access requirement data (e.g., prior authorization, step therapy) allow organizations to better define “the right patients” (i.e., those most likely to encounter access friction) and evaluate impact where access support should matter most. Baseline access conditions can now reflect local payer mix, the level of coverage requirements, and recent experience rather than static market snapshots. These more granular baselines improve confidence that observed prescribing changes are attributable to pull-through efforts rather than underlying access differences.
- Channel spillover: Impactful access engagement may shift broader perceptions of a therapy’s accessibility, influencing prescribing even in patient populations or payer channels where direct engagement has not occurred. Modern measurement approaches increasingly rely on signal-based analytics and granular segmentation across micromarkets and access conditions. These insights help organizations detect spillover effects and link execution across field, digital, and support channels to observed prescribing changes.
- Prescriber perceptions: Access is ultimately an investment in confidence. To realize that value, prescribers must view a therapy as both cost-effective and realistically accessible for their patients. Traditional market research remains important for monitoring these perceptions, but modern analytics provide greater context by linking attitudes to local access conditions, recent prescribing experiences, and funnel-stage friction points. This helps organizations identify which perception shifts matter most for utilization.
Advances in data integration and analytics also allow measurement to occur closer to execution. Shorter feedback loops enable teams to refine targeting, messaging, and support pathways over time, strengthening the effectiveness of pull-through strategies.
Conclusion: Modern pull-through for today’s pharmaceutical access reality
Today’s access environment—shaped by policy and market change, increasing therapeutic complexity, evolving industry operating models, and advances in digital and analytical capabilities—is moving faster than legacy pull-through capabilities can keep up. To remain effective, pull-through must evolve from periodic message delivery to always-on, locally accurate, workflow-ready guidance that is continuously refined as access conditions, provider perceptions, and patient needs change.
Doing so requires a more modern pull-through capability that combines deeper research, clearer local insight, more targeted support, and faster feedback loops across the access journey. AI and modern analytics now make that capability more achievable, helping organizations translate complexity into clearer, more actionable guidance at the point of prescribing.
Organizations that embrace this shift will be better positioned to reduce friction, accelerate time to therapy, and close the gap between access reality and prescriber perception, turning access complexity into more confident prescribing.
1 Berman, M. (2014, February 21). Pull-through capabilities: Communicating effectively with prescribers about cost and coverage [White paper]. Milliman. Retrieved March 11, 2026, from https://www.milliman.com/en/insight/Pull-through-capabilities-Communicating-effectively-with-prescribers-about-cost-and-cover.
2 Lankford, K. (2023, August 2). Milestone moments in Medicare’s history. AARP. Retrieved March 25, 2026, from https://www.aarp.org/medicare/history-of-medicare/.
3 Centers for Medicare and Medicaid Services. (2026, March 16). Selected drugs and negotiated prices. Retrieved March 25, 2026, from https://www.cms.gov/priorities/medicare-prescription-drug-affordability/overview/medicare-drug-price-negotiation-program/selected-drugs-negotiated-prices.
4 Mascarenhas-Melo, F., et al. (2024). An overview of biosimilars—development, quality, regulatory issues, and management in healthcare. Pharmaceuticals, 17(2), 235. Retrieved May 7, 2026, from https://doi.org/10.3390/ph17020235.
5 McCormick, B. (2025, November 25). Patients face new care complexities as DTC options expand. The American Journal of Managed Care. Retrieved March 25, 2026, from https://www.ajmc.com/view/patients-face-new-care-complexities-as-dtc-options-expand.
6 Raza, M. A., Aziz, S., Noreen, M., Saeed, A., Anjum, I., Ahmed, M., & Raza, S. M. (2022). Artificial intelligence (AI) in pharmacy: An overview of innovations. Innovations in Pharmacy, 13(2). Retrieved May 7, 2026, from https://doi.org/10.24926/iip.v13i2.4839.
7 Jirjees, F., Odeh, M., Aloum, L., Kharaba, Z., Alzoubi, K. H., & Al-Obaidi, H. J. (2022). The rise of telepharmacy services during the COVID-19 pandemic: A comprehensive assessment of services in the United Arab Emirates. Pharmacy Practice, 20(2), 2634. Retrieved May 7, 2026, from https://doi.org/10.18549/PharmPract.2022.2.2634.
8 Haydon-Greatting, S. (2022). The era of telehealth pharmacy practice. Journal of the American Pharmacists Association, 62(1), 12–13. Retrieved May 7, 2026, from https://doi.org/10.1016/j.japh.2021.11.027.
9 Knox, S. E., Brennan, C. H., Enright, D. E., Neumann, P. J., & Chambers, J. D. (2026). FDA approvals of specialty drugs, 2000-2024. Health Affairs Scholar, 4(2), qxag035. Retrieved May 7, 2026, from https://doi.org/10.1093/haschl/qxag035.